Dental implants offer a life-changing solution for those with missing teeth, providing a permanent, natural-looking replacement that enhances both the appearance and functionality of your smile. The process of getting dental implants can seem daunting, but with the right preparation and understanding, you can confidently proceed with your treatment. In this article, we’ll walk you through the entire procedure for dental implants, from the initial consultation to the final fitting of your new teeth.
At St Leonards Dental, we are committed to ensuring that your journey to a complete smile is as smooth and comfortable as possible. Whether you’re considering multiple tooth implants or a full mouth restoration, we’ll help you understand each step of the process.
What Are Dental Implants?
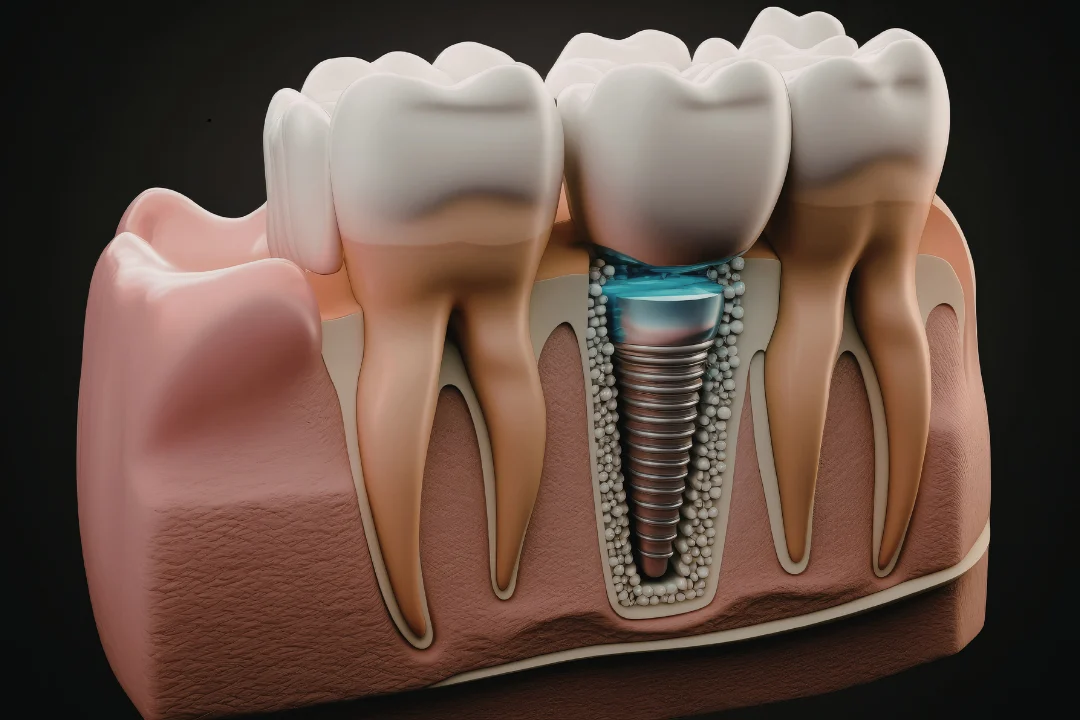
Dental implants are small titanium posts that are surgically inserted into the jawbone to replace the root of a missing tooth. The posts are designed to fuse with the bone over time, providing a stable foundation for the replacement tooth, which could be a crown, bridge, or denture.
What sets dental implants apart from traditional dentures or bridges is their ability to restore both function and appearance with remarkable durability. Implants are biocompatible, meaning they integrate naturally with the bone, providing a long-lasting solution for those who have lost teeth due to decay, injury, or aging.
Why Choose Dental Implants?
Dental implants offer several benefits that make them a preferred choice for many patients:
- Durability and Longevity: With proper care, dental implants can last a lifetime. Unlike dentures, which need to be replaced every few years, implants are a permanent solution.
- Natural Look and Feel: Implants mimic the appearance and function of your natural teeth, allowing you to eat, speak, and smile with confidence.
- Preservation of Jawbone Health: Implants stimulate the jawbone, preventing bone loss that typically occurs when teeth are missing. This helps maintain facial structure and overall oral health.
By choosing dental implants, you’re investing in a solution that improves your quality of life, restores your smile, and supports your long-term dental health.
The Complete Procedure for Placing Dental Implants
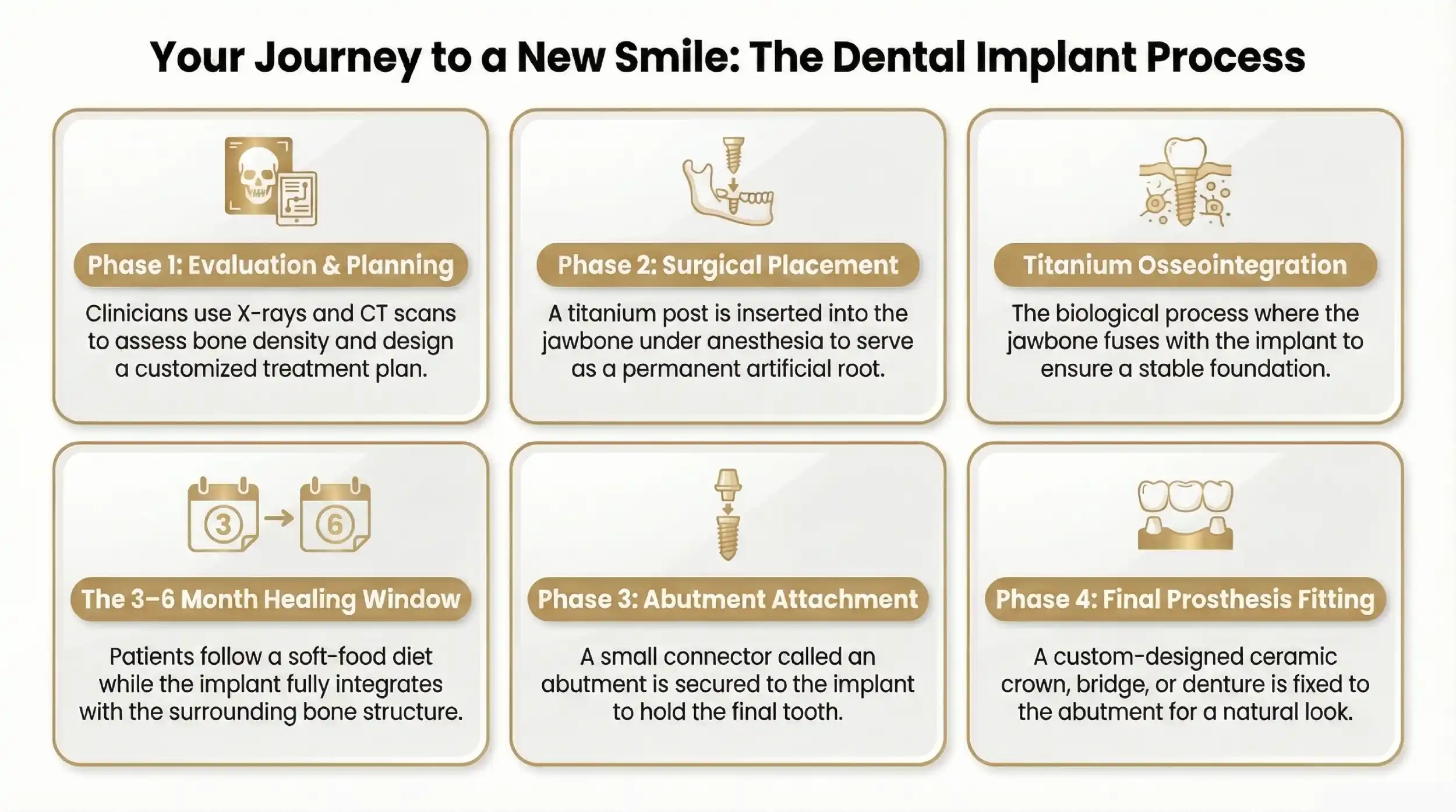
Step 1: Initial Consultation and Evaluation
The first step in the dental implant procedure is the consultation, where your dentist will assess your overall oral health. During this visit, the dentist will:
- Conduct a thorough oral exam to evaluate your gums, teeth, and jawbone.
- Take X-rays or a CT scan to check the condition of your jawbone and determine if you have sufficient bone to support the implant. If you have experienced bone resorption, we may discuss treatment to repair a damaged tooth structure or bone grafting.
- Discuss any underlying medical conditions that could affect the success of the procedure, such as diabetes or osteoporosis.
After assessing your suitability for implants, the dentist will create a personalised treatment plan. If bone loss is detected, you may need bone grafting to strengthen the jawbone before proceeding with implant placement.
Step 2: Treatment Planning and Design
Once your dentist has evaluated your oral health and taken the necessary images, they will design a customised treatment plan. This involves determining:
- The number and location of implants needed.
- The type of prosthesis (crown, bridge, or denture) that best suits your needs.
- Whether any preparatory procedures, like bone grafting or sinus lifts, are necessary to ensure successful implant placement.
By tailoring the plan to your specific needs, your dentist ensures that the procedure will be as effective and comfortable as possible, setting you up for long-term success.
Step 3: Implant Placement Surgery
With your treatment plan in place, the next step is the implant placement surgery. The procedure is done in a sterile environment and typically involves the following steps:
- Anesthesia: Local anesthesia is administered to numb the treatment area. For more complex cases or multiple implants, general anesthesia may be used to keep you comfortable throughout the procedure. Most patients are surprised to find that dental fillings do not hurt more than the actual implant placement, which is performed under profound local anesthesia or sedation.
- Surgical Placement of the Implant: The dentist makes a small incision in the gum to access the jawbone. Once the area is exposed, the titanium post is inserted into the jawbone, acting as the artificial root for the new tooth. If a damaged tooth is still present, a gentle tooth extraction is performed to preserve the surrounding bone.
- Suturing and Initial Recovery: After the implant is securely placed, the gum tissue is sutured back, and the healing process begins. You may experience some swelling and discomfort in the first few days, but these symptoms can typically be managed with medication and ice packs.
Over the next few months, the titanium implant undergoes osseointegration, a process where the bone fuses with the implant. This ensures a stable and permanent foundation for your replacement tooth.
Step 4: Healing and Osseointegration Process
After the implant is placed, it takes several months for the bone to fuse with the titanium post. This process, known as osseointegration, is critical for the long-term success of the implant. During this healing period, you may experience:
- Swelling and discomfort: These are common and can usually be managed with pain medication and ice.
- Follow-up appointments: Your dentist will schedule visits to monitor the healing process and ensure that the implants are integrating properly with the bone.
The healing process typically takes 3 to 6 months, depending on the location and complexity of the implant placement. During this time, you’ll need to follow post-surgery instructions, including:
- Eating soft foods to avoid putting pressure on the healing implant.
- Keeping the surgical site clean to prevent infection.
Once the implant has fully fused with the bone, the healing phase is complete, and you’re ready for the next step: attaching the abutment.
Step 5: Abutment Placement and Final Fitting
After successful healing, the dentist will place a healing abutment on the implant. The abutment is a small connector that protrudes above the gum line and serves as a foundation for the final prosthesis (crown, bridge, or denture). A custom-designed ceramic tooth is fixed to the abutment. This is the stage where we focus on cosmetic dentistry to ensure the new tooth matches your natural smile perfectly. The steps involved include:
- Abutment attachment: The abutment is secured to the implant, and the gums are shaped around it to prepare for the final restoration.
- Impressions and Prosthesis Design: Your dentist will take impressions of your teeth to create a custom prosthesis that matches the shape, colour, and size of your natural teeth.
- Fitting and Adjustments: Once the prosthesis is ready, it is placed onto the abutment. Your dentist will ensure a perfect fit, making any necessary adjustments for comfort and function.
Post-Procedure Care and Maintenance
Proper care after your dental implant procedure is essential to ensure the longevity and functionality of your implants. Here’s what you can expect in the months following your procedure and how to maintain your new smile.
Oral Hygiene
Maintaining proper oral hygiene is crucial for the health of your implants. Brush your implants gently with a soft-bristled toothbrush and use a non-abrasive toothpaste. It’s also important to floss around the implants to remove plaque and food particles. Your dentist may also recommend special cleaning tools, such as an interdental brush or water flosser, to help keep the spaces around the implants clean.
Regular Checkups
After your implants have been placed, regular dental visits are vital. Your dentist will monitor the implants’ health, make sure they are properly integrated into the jaw, and check for any signs of infection or other complications. These checkups will also help ensure the prosthetics (crowns, bridges, or dentures) are still in optimal condition and don’t need adjustments.
Dietary Recommendations
During the healing phase, you will need to follow a soft food diet for a few weeks. After the healing period, you can resume your normal diet, but it’s important to avoid chewing on hard or sticky foods that could damage the implants or prosthetics. Patients often ask why there is no dairy after dental implant surgery; this is to prevent bacterial film (biofilm) from interfering with the initial healing.
Avoid Smoking
Smoking is a significant risk factor for dental implant failure. It can interfere with the healing process, impede osseointegration, and increase the risk of gum disease and infection. It’s highly recommended that you avoid smoking during the healing period and maintain a tobacco-free lifestyle to ensure the success of your implants.
By following these care guidelines, you can maximise the lifespan of your dental implants and enjoy a healthy, functioning smile for many years.
What Complications Can Happen?
Though dental implants are highly successful, there are potential risks and complications that patients should be aware of. While these complications are rare, understanding them can help you stay proactive and vigilant during the recovery process.
Infection
One of the most common risks during the healing process is infection. This can occur if bacteria enter the surgical site or if the area is not cleaned properly. To minimise the risk:
- Maintain excellent oral hygiene to prevent the build-up of plaque and bacteria.
- Follow your dentist’s post-operative care instructions, including taking prescribed antibiotics if needed.
If an infection does occur, it’s typically treated with antibiotics, and in some cases, further surgery may be required to address the issue.
Nerve Damage
Nerve damage is a potential risk during implant placement, particularly in the lower jaw, where nerves are more concentrated. If a nerve is damaged, it can cause numbness, tingling, or pain in the lip, chin, or gums. While nerve damage is rare, it’s more likely to occur in improperly placed implants. Choosing a skilled implant specialist, like the team at St Leonards Dental, significantly reduces this risk.
Sinus Problems
For implants placed in the upper jaw, especially in the back of the mouth near the sinuses, there is a slight risk of sinus issues. If the implant is placed too close to the sinus cavity, it can lead to sinus problems, including infections or discomfort. In some cases, sinus lifts or bone grafting may be performed before implant placement to ensure the sinuses are not affected.
Implant Failure
While rare, implants can fail. This may occur if the implant does not fuse properly with the jawbone (due to insufficient bone density or infection), or if the implant is subject to too much pressure during the healing process. Ensuring proper post-operative care, avoiding stress on the implant site, and adhering to your dentist’s advice can greatly reduce the risk of implant failure.
Alternative Solutions for Tooth Replacement
While dental implants are the preferred option for many, there are other alternatives available for those who may not be candidates for implants or who prefer a different approach. Below are some of the most common alternatives to dental implants:
Dentures: A Removable Option
Dentures are removable appliances that replace missing teeth and restore the function of the mouth. There are two main types of dentures:
- Full dentures: Replace all the teeth in one or both jaws.
- Partial dentures: Replace several missing teeth in a row or in various areas of the mouth.
Pros of Dentures:
- Affordable: Dentures are generally less expensive than implants.
- Non-invasive: Dentures do not require surgery, which makes them a less complex option.
- Immediate use: After the initial fitting, dentures can be used right away.
Cons of Dentures:
- Comfort: Dentures can be uncomfortable and may slip while eating or speaking.
- Maintenance: Dentures require ongoing adjustments and cleaning, and they need to be replaced every few years.
- Bone Loss: Dentures do not help prevent bone loss in the jaw, which can change the shape of the face over time.
Although dentures provide an option for those with missing teeth, they do not offer the same level of comfort, stability, and bone preservation that dental implants do.
Dental Bridges: A Fixed Option for Missing Teeth
A dental bridge is a fixed prosthetic that replaces one or more missing teeth. The bridge is anchored to the remaining natural teeth on either side of the gap, or it can be supported by implants.
Pros of Dental Bridges:
- Fixed solution: Unlike dentures, dental bridges are fixed in place, which means there is no need to remove them for cleaning.
- Restores Function: Dental bridges restore the ability to chew and speak properly, much like implants.
Cons of Dental Bridges:
- Damage to Adjacent Teeth: In traditional bridges, the healthy teeth on either side of the gap need to be reshaped to accommodate the bridge, which can damage them over time.
- Shorter Lifespan: Dental bridges do not last as long as dental implants and may need to be replaced every 10-15 years.
For those with several missing teeth in a row, dental bridges offer a good alternative to implants, but they don’t provide the same level of stability or bone preservation.
Frequently Asked Questions (FAQs)
How Long Do Dental Implants Last?
Dental implants are designed to be permanent and, with proper care, can last 20 years or more. The crown or prosthesis may need to be replaced after 10-15 years, but the titanium post typically lasts a lifetime.
Can Anyone Get Dental Implants?
Most healthy individuals who have sufficient bone density in the jaw are good candidates for dental implants. If you have bone loss, procedures like bone grafting may be necessary to ensure success. A thorough evaluation by a skilled implant specialist is essential.
What Happens if I Don’t Have Enough Bone for Implants?
If you lack sufficient bone for implants, bone grafting can help rebuild the bone in the jaw, providing a stable foundation for the implants. Alternatively, Zygomatic implants may be used for patients with severe bone loss.
How Much Do Dental Implants Cost?
The cost of dental implants can vary based on factors like the number of implants required, the type of prosthesis, and whether additional procedures like bone grafting are needed. On average, dental implants can range from $3,000 to $6,000 per implant.
Are There Risks of Implant Failure?
Though rare, implant failure can occur if the implant does not fuse with the bone or if there is infection. Regular checkups and proper care help minimise the risk of failure.
Conclusion: Restore Your Smile with Confidence
Dental implants are a reliable and long-lasting solution for restoring missing teeth. Whether you’re considering multiple tooth implants or full mouth restoration, St Leonards Dental is here to guide you through every step of the procedure. From the initial consultation to post-operative care, we’re committed to helping you achieve a beautiful, functional smile. Contact us today to schedule your consultation and start your journey toward a healthier, more confident smile!