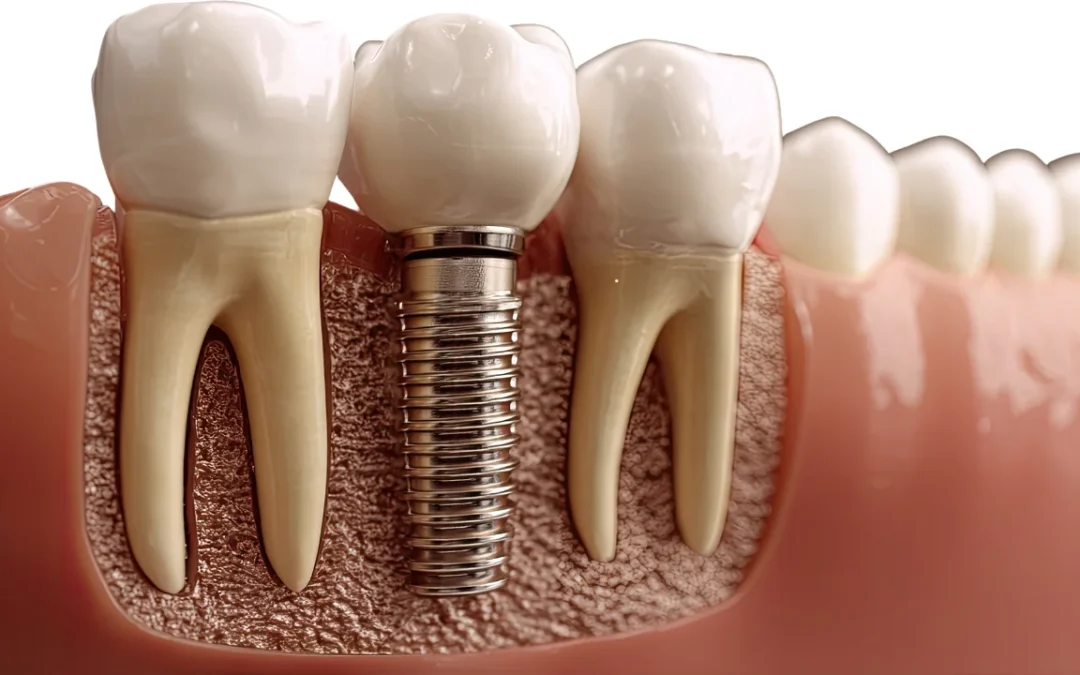
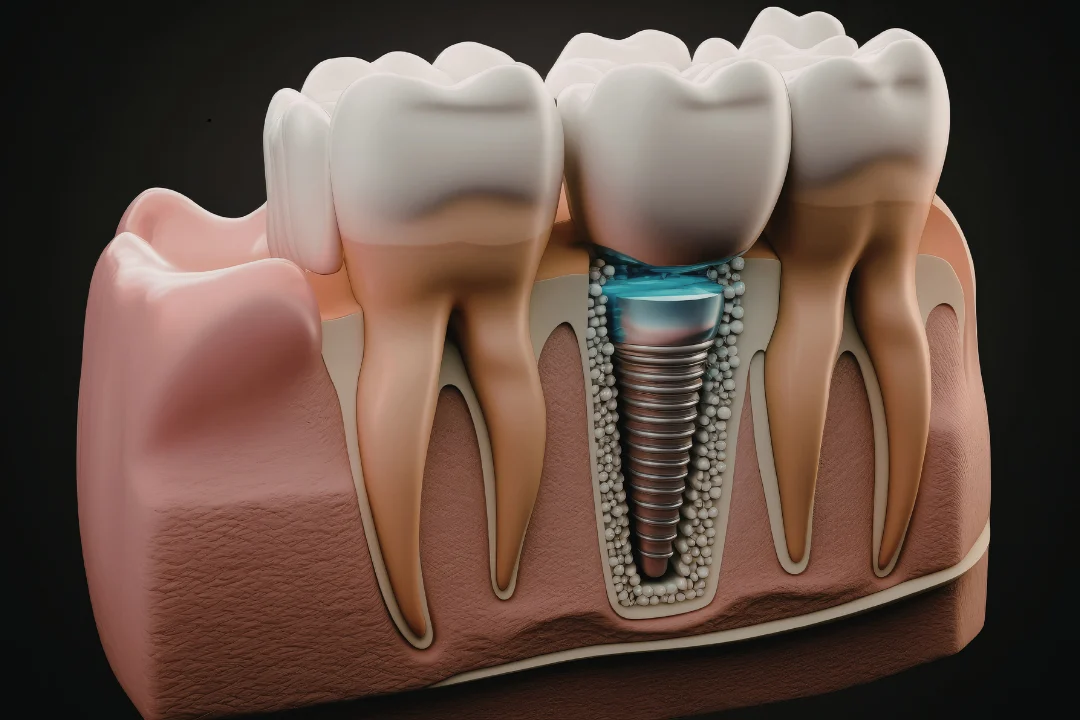
Dental implants are an effective way to restore missing teeth, offering strength, stability, and a natural look. However, like any surgical procedure, they come with risks, the most serious of which is dental implant infection. If left untreated, infections can lead to peri-implantitis, bone loss, or even failure of the implant. For patients in Australia, particularly around Sydney and St Leonards, understanding how infections develop, their warning signs, and how to treat them is crucial. At St Leonards Dental, we provide comprehensive care that ensures your implants remain healthy and functional for years. This guide addresses everything you need to know to prevent, identify, and manage implant infections effectively.
What is a Dental Implant Infection?
A dental implant infection occurs when harmful bacteria accumulate around the implant, leading to gum inflammation and, in more serious cases, bone loss around the implant site. There are two main conditions that dentists monitor:
- Peri-implant mucositis: This is an early-stage infection affecting only the soft tissues around the implant. The gums may appear red and swollen and bleed during brushing or flossing. This condition is reversible if caught early with proper non-surgical treatments, including professional cleaning and improved hygiene practices.
- Peri-implantitis: When the infection progresses beyond the soft tissues into the supporting bone, it is termed peri-implantitis. This condition can lead to implant mobility, pain, and eventual implant failure if not treated promptly. Symptoms often include swelling, pus discharge, gum recession, and a foul taste or odor in the mouth. Detecting peri-implantitis early is essential for preserving both the implant and the surrounding bone structure.
Dental professionals use specialised dental instruments and scaling tools to assess and clean the affected areas. In more severe cases, surgical interventions such as flap surgery or bone grafting may be necessary to restore oral health.
How Common Are Dental Implant Infections?
While dental implants have a high success rate in Australia, studies show that up to 20% of patients may develop peri-implant mucositis, and around 10% may experience peri-implantitis over the long term. Risk factors like smoking, poor oral hygiene, diabetes, and a history of gum disease significantly increase the likelihood of infection. Even patients who maintain excellent care may experience late-onset infections years after implantation, highlighting the importance of regular check-ups and monitoring for early symptoms. Using antiseptic mouthwash, regular cleaning, and dental tools for scaling and debridement, we work to maintain implant stability and prevent bone loss before it becomes a serious problem.
What Causes Dental Implant Infections?
Understanding the root causes of dental implant infection can help you avoid complications and protect your oral health. The primary contributors include:
- Bacterial Plaque & Biofilm Accumulation
Plaque is a sticky film of bacteria that naturally forms in the mouth. When it builds up around implants, it can lead to gum inflammation, peri-implant mucositis, and eventually peri-implantitis if untreated. - Poor Oral Hygiene
Skipping daily brushing or flossing allows bacteria to accumulate. Using a soft-bristled brush, floss, and antiseptic mouthwash is essential to prevent infections. - Systemic Health Conditions
Patients with diabetes, autoimmune disorders, or a weakened immune system are more susceptible to infections, as their body’s ability to fight bacteria is compromised. - Lifestyle Factors
Smoking and excessive alcohol use significantly increase the risk of implant infection. Smoking reduces blood flow to the gums and slows healing. - Surgical or Prosthetic Factors
Implant placement errors, residual cement under the gums, excessive bite force on the implant, or irregular professional maintenance can create conditions conducive to bone loss and peri-implantitis. - History of Gum Disease
Patients with prior periodontal disease may have residual bacteria that can attack a newly placed implant if precautions are not taken.
By addressing these causes through preventive measures, professional dental care, and lifestyle adjustments, patients in Australia can reduce their risk of infection and maintain implant health for the long term.
Signs & Symptoms of Dental Implant Infection
Recognising the early warning signs of a dental implant infection is critical for preventing peri-implantitis and bone loss. Patients often notice subtle changes that can escalate if ignored. Common symptoms include:
- Redness and Swelling: Inflamed gums around the implant, often tender to the touch, indicate gum inflammation. Early redness can progress to a more serious infection if untreated.
- Pain or Discomfort: Mild to moderate pain may occur around the implant site. Persistent or throbbing pain suggests deeper tissue involvement.
- Bleeding or Pus Discharge: Gums may bleed during brushing or flossing. The presence of pus is a strong indicator of peri-implantitis, which requires immediate attention.
- Bad Taste or Foul Odor: Bacterial activity around the implant can produce an unpleasant taste or smell in the mouth.
- Mobility of the Implant: Loosening or movement of the dental implant may indicate that the supporting bone is compromised.
- Gum Recession: Gradual exposure of the implant or abutment due to receding gum tissues.
- Fever or General Malaise: In rare cases, systemic infection may occur if the implant infection is severe.
Common Symptoms, Severity, and Recommended Actions
| Symptom | Severity | Recommended Action | Expected Outcome |
| Redness & Swelling | Mild to Moderate | Antiseptic rinse, professional cleaning | Reduces inflammation, prevents progression |
| Pain | Mild to Severe | Pain management, non-surgical cleaning, antibiotics | Relief from discomfort, infection control |
| Pus / Discharge | Moderate to Severe | Surgical debridement, antibiotics | Infection resolution, implant retention |
| Gum Recession | Moderate | Professional monitoring, bone graft if necessary | Preservation of implant & surrounding bone |
| Loose Implant | Severe | Surgical correction or implant replacement | Implant replacement if necessary, restores function |
| Bad Taste / Foul Odor | Mild to Moderate | Improved hygiene, antiseptic mouthwash | Resolves odor, controls infection |
At St Leonards Dental, we emphasise early detection of these symptoms. Our team conducts thorough evaluations using dental instruments, scaling tools, and radiographic imaging to identify the stage of infection and determine the appropriate treatment.
Diagnosis of Dental Implant Infection
Proper diagnosis is essential to determine whether the implant infection is peri-implant mucositis or peri-implantitis, and to decide the treatment pathway. Key diagnostic steps include:
- Clinical Examination: Dentists assess gum color, swelling, bleeding, and mobility of the implant. Probing depths around the implant helps detect pocket formation and tissue inflammation.
- Radiographic Imaging: X-rays or 3D imaging identify bone loss around the implant. Early bone changes are sometimes not visible without professional imaging, making regular check-ups essential.
- Assessment of Risk Factors: Smoking history, diabetes, oral hygiene habits, and prior periodontal disease are evaluated to understand the infection’s root cause.
- Symptom Monitoring: Patients are asked to report pain, swelling, pus, bleeding, or bad taste to identify the infection stage early.
Accurate diagnosis ensures that treatments, whether non-surgical or surgical, are effective and targeted, maximising the chance of implant retention and restoration of bone structure.
Treatment Options for Dental Implant Infection
Treatment depends on the severity of the infection and whether it is limited to soft tissue (peri-implant mucositis) or involves the bone (peri-implantitis). We offer a full range of interventions to resolve infections and preserve implant health.
Non-Surgical Treatments
For early or mild infections, non-surgical treatments are often sufficient to restore oral health:
- Professional Cleaning and Scaling: Removal of plaque and tartar using specialised dental instruments and scaling tools.
- Antibiotic Therapy: Localised or systemic antibiotics target bacterial growth and help control infection.
- Antiseptic Mouthwash: Chlorhexidine or similar antiseptic rinses reduce bacterial load around the implant.
- Improved Oral Hygiene: Daily brushing, flossing, and interdental cleaning reduce biofilm accumulation and prevent recurrence.
These treatments are highly effective for peri-implant mucositis, helping to reverse gum inflammation, relieve pain, and prevent bone loss.
Surgical Treatments
When infection progresses to peri-implantitis with bone involvement, surgical interventions are required:
- Flap Surgery: Accessing the infected area to thoroughly clean bacterial deposits and debride affected tissues.
- Bone Grafting: Using bone graft material to restore lost bone structure and support the implant.
- Implant Removal and Replacement: In severe cases where the implant is loose or bone destruction is significant, removing the implant and planning re-implantation is necessary.
Table: Severity-Based Treatment Overview
| Infection Stage | Treatment Approach | Expected Outcome |
| Mild (Peri-implant mucositis) | Non-surgical cleaning, mouthwash, and antibiotics | Infection resolution, implant retention |
| Moderate | Deep cleaning, localised antibiotic therapy | Pain relief, infection control, and prevents bone loss |
| Severe (Peri-implantitis) | Flap surgery, bone grafting, and possible implant replacement | Restoration of bone structure, implant stability |
At St Leonards Dental, all treatments are performed with the latest dental instruments and materials, ensuring patient comfort and maximising the chance of implant retention and infection resolution.
Preventing Dental Implant Infection
Preventing a dental implant infection is far easier than treating one. Patients can maintain healthy implants for life by following consistent care routines and professional guidance. Key preventive strategies include:
- Daily Cleaning: Brush your teeth at least twice a day using a soft-bristled toothbrush to gently clean around implants. Ensure you reach all surfaces to remove bacterial plaque.
- Flossing and Interdental Cleaning: Use implant-specific floss or interdental brushes to clean between teeth and around the implant, preventing gum inflammation and peri-implant mucositis.
- Antiseptic Mouthwash: Rinse with an antiseptic mouthwash like chlorhexidine to reduce bacterial load and protect against infection.
- Regular Professional Check-Ups: Schedule dental visits every 6–12 months for professional cleaning, examination, and early detection of any infection. Our team at St Leonards Dental uses advanced dental instruments and scaling tools to ensure thorough maintenance.
- Avoid Smoking: Tobacco use reduces blood flow to gums and slows healing, making implants more vulnerable to peri-implantitis.
- Manage Health Conditions: Control systemic factors like diabetes, osteoporosis, and autoimmune conditions, which increase susceptibility to infection.
By adhering to these measures, patients can reduce the risk of bone loss, gum inflammation, and implant failure, while maintaining overall oral health.
When to Seek Urgent Dental Care
Even with careful prevention, infections can occur. Prompt action is critical to prevent complications. Contact your dentist immediately if you notice:
- Persistent swelling or redness around the implant
- Pain or throbbing discomfort that does not improve with normal care
- Pus, discharge, or foul taste/odor
- Loose or mobile implant
- Bleeding gums that persist despite good hygiene
- Fever or general illness accompanying oral symptoms
We provide same-day appointments for patients experiencing implant complications. Early intervention with non-surgical treatments or surgical procedures ensures the best outcomes, including infection resolution, pain relief, and preservation of implant stability. Often asked, “How long do dental implants last?” A dental implant fuses with your jawbone and becomes a permanent part of your mouth, often lasting for decades.
The Importance of Professional Maintenance
Regular professional maintenance plays a critical role in preventing peri-implantitis and ensuring long-term implant success. Our dental team monitors:
- Implant stability and bone levels using radiographic imaging
- Gum health, checking for inflammation, bleeding, and early infection signs
- Proper prosthetic fit to prevent excessive force or cement residue that can cause infection
Professional intervention helps preserve the implant, restore bone structure, and avoid complex surgical procedures in the future. Ongoing guidance on daily hygiene, risk factor management, and lifestyle choices ensures that your dental implants remain healthy and functional.
Final Thought
Dental implant infections, including peri-implant mucositis and peri-implantitis, are serious conditions that require careful attention. By understanding causes, symptoms, risk factors, and treatment options, patients can protect their oral health and preserve their dental implants.
At St Leonards Dental, we provide comprehensive care tailored to the needs of patients in St Leonards and across New South Wales. From early detection and non-surgical cleaning to surgical interventions like flap surgery and bone grafting, our team ensures effective infection resolution, implant retention, and restoration of bone structure. With proper daily hygiene, regular check-ups, and professional maintenance, you can enjoy the full benefits of dental implants with confidence and peace of mind.
For personalised advice or to schedule a consultation, contact us at St Leonards Dental today. Our experienced dentists are ready to help prevent and treat dental implant infections, keeping your smile healthy and strong.