Many people consider dental implants the best long-term solution for missing teeth, but smoking can quietly reduce their success. If you smoke or vape, your risk of implant failure increases significantly, even if everything else is done correctly. This creates a common problem: patients invest in implant treatment but face complications such as slow healing, infections, or even implant loss. The good news is that these risks can be managed with the right steps before and after surgery. In this guide, you will learn how smoking affects dental implants, what the real risks are, and how to improve your chances of success. If you are planning treatment in Australia, clinics like St Leonards Green Dental offer personalised implant consultations to help patients reduce these risks early.
Dental Implants Explained: What Needs to Happen for Success
A dental implant is a small titanium post placed into the jawbone to act as an artificial tooth root. Once healed, it supports a crown, bridge, or even full mouth restoration. Titanium is used because it is biocompatible, meaning the body accepts it without rejection. Implants are widely used across Australia because they look natural, restore chewing ability, and help maintain bone structure after tooth loss. At St Leonards Green Dental, patients can receive complete implant solutions, from single tooth replacement to full mouth restorations.
Osseointegration: The Most Important Healing Stage
Osseointegration is the process by which the jawbone fuses with the implant surface. This stage determines whether the implant will stay stable for years. After placement, bone cells called osteoblasts attach to the titanium surface and begin forming new bone around it. This process depends heavily on blood supply, oxygen, and healthy tissue. Smoking interferes with all of these factors. Nicotine reduces blood flow, which limits oxygen reaching the healing area. As a result, bone bonding becomes weaker, increasing the chance of implant loosening or failure.
Normal Success vs Failure Rates
Dental implants generally have high success rates, but smoking changes these outcomes significantly. According to the American Academy of Implant Dentistry, implants have a success rate of up to 98% in healthy individuals. However, research shows that smokers face much higher risks.
| Patient Type | Success Rate | Failure Risk |
| Non-smokers | 94–98% | 1–3% |
| Light smokers | 90–95% | 5–10% |
| Heavy smokers | 70–85% | Up to 30% |
Studies referenced by the National Institutes of Health indicate that smokers can be up to 2.4 times more likely to experience implant failure compared to non-smokers. This shows why smoking is considered one of the biggest risk factors in implant dentistry.
How Smoking Disrupts Implant Healing
To understand why smoking causes implant problems, it helps to look at what happens inside the body during healing. Smoking affects blood circulation, bone cells, and the immune system. These changes make it harder for the implant to bond with the jawbone and increase the chance of complications.
Nicotine and Blood Flow Restriction
Nicotine causes blood vessels to narrow, which reduces blood flow to the gums and jawbone. This limits the delivery of oxygen and nutrients needed for healing. It also increases blood thickness, making circulation less efficient. Reduced blood flow slows healing and increases the risk of infection after surgery. For dental implants, this means the surrounding tissues may not recover properly, leading to early failure.
Impact on Bone Cells and Osseointegration
Smoking directly affects the activity of bone-forming cells. Osteoblasts become less active, while bone-resorbing cells increase, leading to bone loss instead of bone growth. This weakens the bond between the implant and the jawbone. Over time, this can cause the implant to loosen. This is one of the main reasons smokers experience higher failure rates, especially in areas like the upper jaw (maxilla), where bone density is already lower.
Effect on Soft Tissue and Immune Response
Smoking also weakens the body’s ability to fight infection. The immune system becomes less effective, allowing bacteria to grow more easily around the implant. This can lead to inflammation of the peri-implant tissues, known as peri-implantitis. Gum tissue may heal slowly, remain swollen, or become infected. Smoking is a major risk factor for gum disease, which further increases implant complications.
Smoking & Dental Implants: Real Clinical Risks and Complications
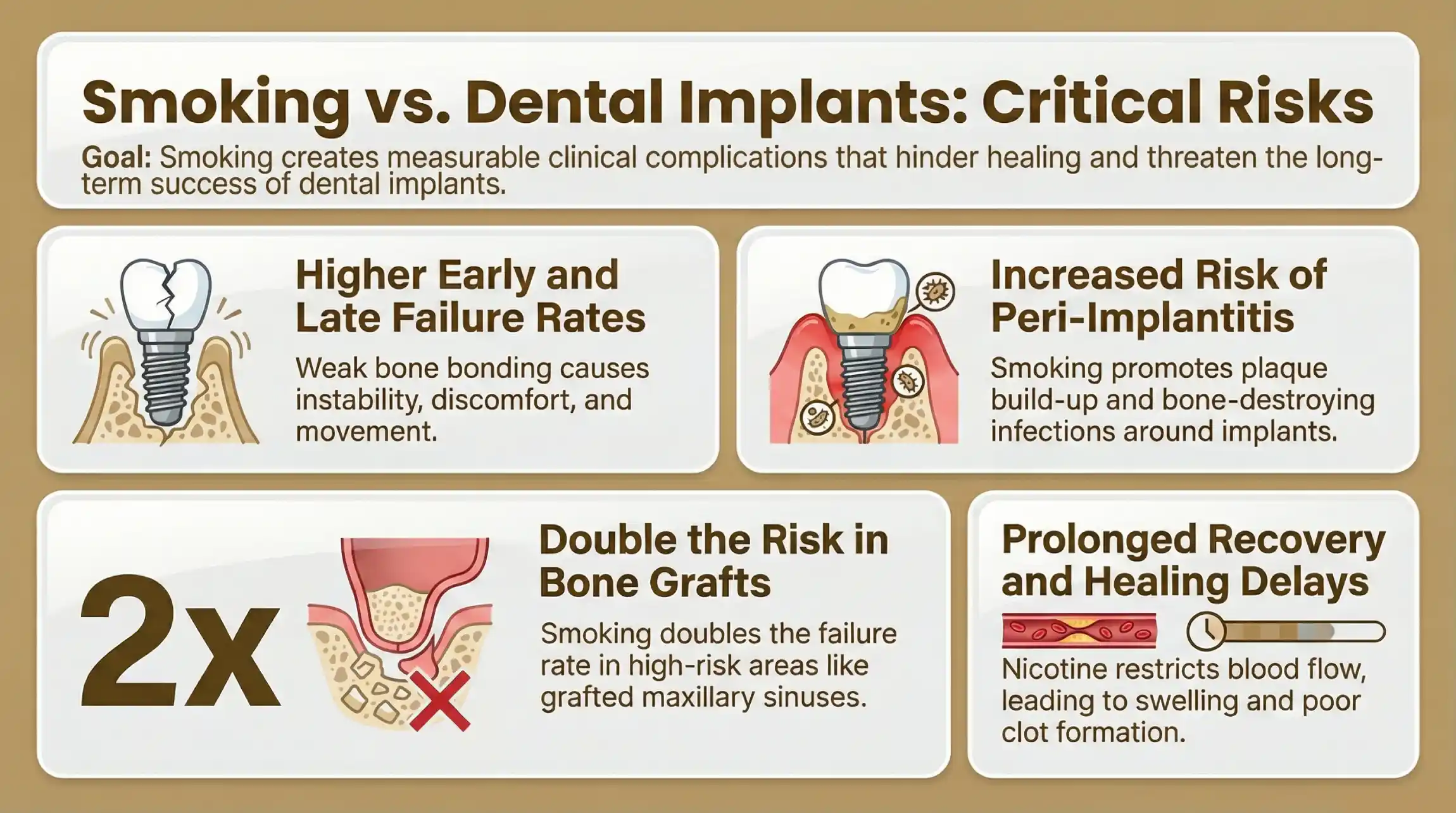
Smoking does not just affect healing it leads to real, measurable complications that can impact both short-term recovery and long-term implant stability. Understanding these risks helps patients make informed decisions before starting treatment.
Dental Implant Failure and Loosening
Implant failure can happen early, before the implant fully integrates, or later, after it has been in place for some time. In smokers, weak bone bonding often causes the implant to become unstable. This may result in discomfort, movement, or complete failure. According to clinical studies cited by the National Institutes of Health, smokers have significantly higher early failure rates due to poor healing conditions.
Peri-Implantitis and Gum Disease Around Implants
Peri-implantitis is an infection that affects the gum and bone around an implant. It is similar to gum disease but occurs around implants instead of natural teeth. Smoking increases plaque build-up and reduces the body’s ability to fight bacteria. This leads to inflammation, bleeding, and gradual bone loss. If untreated, peri-implantitis can cause implant failure.
Delayed Healing and Surgical Complications
After implant surgery, smokers often experience a slower recovery. This includes prolonged swelling, discomfort, and higher chances of complications such as dry socket or poor blood clot formation. Healing delays can extend treatment time and increase the need for additional procedures. Clinics like St Leonards Green Dental provide guided post-operative care to help reduce these risks and support proper healing.
Bone Loss and Failure in High-Risk Areas
Bone loss is one of the most serious complications linked to smoking. It occurs more frequently in the upper jaw (maxilla) than in the lower jaw (mandible). This is because the upper jaw naturally has softer bone. In cases where bone grafts or grafted maxillary sinuses are used, smoking can double the failure risk. This makes careful planning and smoking cessation even more important for successful outcomes.
Smoking Intensity and Risk Levels
Not all smokers face the same level of risk, but even small amounts of smoking can affect dental implant success. Research shows a clear pattern: the more frequently a person smokes, the higher the chance of complications. This happens because repeated exposure to nicotine and tobacco chemicals keeps reducing blood flow, slowing healing, and weakening bone support. For patients considering implants in Australia, understanding where they fall on this risk scale can help guide better decisions before treatment begins.
Light vs Heavy Smokers
Smoking intensity is usually measured by the number of cigarettes consumed daily. Light smokers typically smoke between 1–10 cigarettes per day, while heavy smokers exceed 10 cigarettes daily. Even light smokers face a noticeable increase in implant failure risk compared to non-smokers. However, heavy smokers experience the highest complication rates, including infections, delayed healing, and implant loosening. According to studies referenced by the National Institutes of Health, heavy smokers can face failure rates of up to 30%, which is significantly higher than those of non-smokers.
Dose-Response Relationship
There is a direct link between smoking frequency and implant failure. This is known as a dose-response relationship. The more cigarettes smoked, the greater the exposure to harmful chemicals like nicotine and carbon monoxide. These substances reduce oxygen levels in the blood and interfere with bone healing. Research indicates that smokers may have up to a 140% higher risk of implant complications compared to non-smokers. This is why dentists strongly recommend reducing or quitting smoking before undergoing implant surgery.
Social Smoking Still Carries Risk
Many people assume occasional or social smoking is harmless, especially if it is limited to weekends or social events. However, even small amounts of smoking during the healing phase can disrupt osseointegration. The early weeks after implant placement are critical, and any exposure to nicotine during this period can interfere with bone bonding. This means that even infrequent smoking can increase the chance of implant failure.
Vaping, Nicotine Products, and Hidden Risks
As smoking habits change, many patients switch to vaping or nicotine replacement products, believing they are safer alternatives. While these options may reduce exposure to some harmful chemicals, they still pose risks for dental implant success. Understanding these risks is important for making informed decisions during treatment planning.
Is Vaping Safer for Dental Implants?
Vaping is often seen as a safer option than traditional cigarettes, but it still exposes the mouth to heat, chemicals, and nicotine. These factors can irritate gum tissue and reduce healing capacity. Although vaping may produce less tar, it still affects blood flow and increases inflammation in the gums. This means it can still interfere with osseointegration and increase the risk of implant complications. Beyond nicotine, your immediate post-op diet is crucial; understanding why no dairy after dental implant surgery is recommended can help prevent bacterial film from forming near the healing site.
Nicotine Replacement Therapy (NRT)
Nicotine replacement products such as patches, gums, and lozenges are commonly used to help people quit smoking. These options remove harmful smoke toxins but still deliver nicotine into the body. While they are generally safer than smoking, nicotine itself can still restrict blood flow and slow healing. Dentists may allow controlled use of NRT during the quitting process, but reducing nicotine intake completely during the healing phase offers the best results.
Alcohol, Diet, and Lifestyle Factors
Smoking is often linked with other habits that can affect implant success. Alcohol consumption can slow healing and increase inflammation. Diets high in sugar, junk food, and fizzy drinks can lead to plaque build-up and gum disease, which further increases the risk of peri-implantitis. Maintaining a balanced diet, staying hydrated, and reducing alcohol intake can support better healing outcomes. At St Leonards Green Dental, patients receive guidance on lifestyle changes that support long-term implant success.
The Critical Quit Timeline for Implant Success
Timing plays a major role in reducing implant risks for smokers. Quitting at the right time allows the body to recover and improves healing conditions. Many patients ask how long they need to stop smoking before and after implant surgery, and the answer depends on the healing process.
Before Implant Surgery
Stopping smoking before surgery helps improve blood circulation and oxygen levels in the body. Ideally, patients should quit at least 2 to 8 weeks before surgery. Even stopping 1 week before can provide some benefit by improving blood flow and reducing complications during the procedure. Dentists often assess smoking history during consultations and may recommend delaying treatment until conditions improve.
After Implant Placement
The period after surgery is the most critical. During this time, the implant begins bonding with the bone. Smoking during this stage can interrupt healing and increase failure risk. Patients are advised to avoid smoking for at least 2 to 3 months after implant placement. This allows osseointegration to occur without interference from nicotine or toxins.
Why This Window Matters
The early healing phase is when the implant becomes stable. Blood clot formation, bone growth, and tissue repair all happen during this time. Smoking disrupts each of these processes. According to clinical guidance referenced by the Mayo Clinic, avoiding smoking during this window significantly improves healing outcomes and reduces complications.
Patient Evaluation: How Dentists Assess Smokers Before Implants
Before recommending dental implants, dentists carefully evaluate each patient’s health and lifestyle. For smokers, this step is essential to identify risks and plan treatment accordingly. A thorough assessment helps improve success rates and reduces the chance of complications.
Medical and Smoking History
Dentists begin by reviewing the patient’s smoking habits, including how long they have smoked and how frequently. This helps determine whether they fall into a light or heavy smoking category. Medical conditions such as diabetes, heart disease, or lung issues are also considered, as these can further affect healing.
Oral Health and Bone Assessment
A detailed examination of the mouth is performed to check gum health, bone density, and any signs of infection. X-rays or 3D scans may be used to evaluate the jawbone, especially in areas like the maxilla where bone is softer. If bone loss is present, additional procedures such as bone grafts may be recommended before implant placement.
Risk-Based Treatment Planning
Based on the findings, dentists create a personalised treatment plan. This may include recommending smoking cessation, improving oral hygiene, or scheduling additional procedures to strengthen the jawbone. At St Leonards Green Dental, patients receive tailored dental implant planning that considers lifestyle factors like smoking, ensuring safer and more predictable outcomes.
How to Improve Implant Success as a Smoker
Even if you currently smoke, there are practical steps you can take to improve your chances of a successful dental implant. The key is to support your body before, during, and after the procedure so healing can happen properly. Many implant failures can be avoided when patients follow the right preparation and aftercare plan.
Pre-Surgery Preparation
Preparing your body before implant surgery plays a major role in the final outcome. Reducing or stopping smoking is the most important step. Even a short break can improve blood circulation and oxygen levels. Along with this, a professional dental cleaning helps remove plaque and tartar, reducing bacterial load in the mouth. Dentists may also prescribe medications such as antibiotics to control infection risk before surgery.
Surgical Considerations
In some cases, dentists may adjust the treatment approach for smokers to improve success rates. This can include using advanced implant surfaces such as hydroxyapatite-coated implants, which help promote better bone attachment. If the jawbone is weak, procedures like bone grafting may be required to create a stable foundation. These techniques are especially important in areas like the upper jaw, where bone density is naturally lower.
Early Healing Protection
The first few weeks after surgery are critical. During this time, the implant begins bonding with the bone. Avoiding smoking completely during this stage is essential. Patients should also follow all post-operative instructions, including maintaining oral hygiene, using prescribed mouth rinses, and attending follow-up visits. Protecting the implant during this early phase greatly increases long-term success.
Long-Term Implant Care for Smokers
After the implant has healed, ongoing care becomes essential to maintain its stability. Smokers need to be extra careful because their risk of gum disease and infection remains higher compared to non-smokers.
Daily Oral Hygiene Routine
Maintaining a consistent oral hygiene routine helps prevent plaque build-up around the implant. This includes brushing twice daily with fluoride toothpaste and cleaning between teeth using interdental brushes or water flossers. These tools are especially useful for reaching areas around implants that regular brushing may miss.
Preventing Peri-Implant Disease
Peri-implantitis is one of the leading causes of implant failure in smokers. It starts with inflammation and can progress to bone loss if untreated. Using antimicrobial mouth rinses and keeping the gum area clean can reduce bacterial growth. Regular hygiene visits also help remove plaque before it causes damage. Because smoking masks bleeding, a primary sign of infection, patients must be vigilant for other signs of tooth abscess or localized inflammation that could signal peri-implantitis.
Monitoring Signs of Complications
Patients should watch for early warning signs such as bleeding gums, swelling, persistent bad breath, or any movement in the implant. These symptoms may indicate infection or bone loss. Early treatment can prevent more serious issues. At St Leonards Green Dental, ongoing maintenance programs help patients monitor and protect their implants over time.
Are Dental Implants the Right Choice for Smokers?
Choosing dental implants as a smoker requires careful consideration. While implants are still possible, the risks are higher, and success depends on lifestyle changes and proper care.
When Implants Are Still Viable
Smokers may still be suitable candidates if they reduce or quit smoking, maintain good oral hygiene, and have strong bone density. Regular dental visits and proper care can help improve outcomes. Many patients successfully receive implants after making these adjustments.
When Risk May Be Too High
In some cases, the risks may outweigh the benefits. Heavy smokers, patients with severe gum disease, or those with poor healing ability may face a higher chance of implant failure. Dentists may recommend alternative treatments in these situations to avoid complications.
Frequently Asked Questions (FAQs)
Can smokers get dental implants successfully?
Yes, but the risk of failure is higher. Success depends on reducing smoking, maintaining good oral hygiene, and following professional advice.
How long should I quit smoking before implants?
It is recommended to stop at least 1–2 weeks before surgery, with longer periods offering better outcomes.
Is vaping safer than smoking for implants?
No, vaping still affects healing due to nicotine and chemical exposure.
What happens if I smoke after implant surgery?
Smoking can delay healing, increase infection risk, and lead to implant failure.
Do implants fail more in the upper jaw?
Yes, especially in smokers, because the upper jaw has softer bone and lower density.
Can gum disease from smoking affect implants?
Yes, gum disease increases the risk of peri-implantitis and implant failure.
Conclusion: Making a Safe and Informed Decision
Smoking has a clear and proven impact on dental implant success. It affects healing, increases infection risk, and raises the chance of implant failure. However, with the right steps, many of these risks can be reduced. Quitting smoking, even temporarily, can significantly improve outcomes. Proper planning, professional care, and long-term maintenance all play an important role in achieving successful results. If you are considering dental implants, booking a consultation with St Leonards Green Dental can help you understand your options and create a personalised plan for a healthier, more confident smile.
References
American Academy of Implant Dentistry (AAID)
National Institutes of Health (NIH) / PMC